↱ 16.9% = 65+
In fact, older Canadians account for at least 45% of all health care spending, 42% of hospitalizations and 59% of all hospital days. The demographic challenge facing our health care system is compounded by the fact that our older population is set to double in the coming two decades.
The changing needs and priorities of our ageing population are challenging us to shift our thinking in how we conceptualize and provide care. It is becoming clearer than ever that older patients require more integrated responses to their care needs from our health care system and greater support to enable healthy ageing in the first place.
As health care providers, we need to develop more innovative ways to treat our older patients as individuals, and not as a series of isolated issues, while also supporting their families and caregivers. Innovation in the fields of healthy ageing and geriatrics further requires a proactive, interprofessional and team-based approach to deliver comprehensive and integrated care across the entire continuum of care.
Healthy Ageing and Geriatrics as a Core Priority
In 2010, Mount Sinai Hospital became the first acute care academic health sciences centre in Canada to make healthy ageing and geriatrics a core strategic priority. Now that Mount Sinai Hospital has become part of the larger Sinai Health, the understanding that healthy ageing requires a more holistic approach to the care of older adults resonates across our entire organization that is now even better designed to treat and manage the care of older patients. From how we deliver care to how we design our spaces, healthy ageing and geriatrics is now at the core of what we do across Sinai Health.
Acute Care for Elders (ACE) Strategy
Sinai Health’s award-winning Acute Care for Elders (ACE) Strategy was launched in 2010 to improve how we deliver care to older patients. Our organization, under this strategy, continues to develop, implement and link together a series of evidence-informed models of care and best practices to create a more integrated experience for older patients, their families, and caregivers across the continuum of care. We are proud that we are being supported by the federally funded Canadian Foundation for Healthcare Improvement (CFHI) and the Canadian Frailty Network (CFN) to help others implement our ACE Strategy in communities across Canada and around the world.
Overall, our ACE Strategy aims to improve the care we provide based around four overall principles:
- We seek to redesign or establish new sustainable approaches that enhance and improve upon current service delivery models.
- We seek to shift the traditional thinking that currently underpins the administration and culture of most traditional care organizations.
- We identify risk factors and needs, and intervene early to support and maintain an older person’s independence.
- We are committed to maintaining a relentless focus on monitoring and evaluating our outcomes to continuously improve the work we carry out.
Between 2010 and 2015, Mount Sinai Hospital experienced a 53.4% increase in hospital admissions among adults aged 65 and older largely due to the fact that Toronto’s downtown population is growing and ageing rapidly. Nevertheless, Mount Sinai has maintained the region’s lowest admission rate of older patients to hospital at 25% which is 18% lower than the regional admission rate of 31%. For those patients who are admitted to hospital, our ACE Strategy has facilitated significant changes in our traditional care processes across the hospital that has helped to achieve a remarkable 25.8% decrease in the average length of stay, and a 14% decrease in readmissions to our hospital among our patients aged 65 and older. Our improved efficiencies are largely linked to the improved quality of care we are providing to our older patients that has resulted in a 50% decrease in the use of urinary catheters, a 66% decrease in our rates of falls in hospital, and an astonishing 93% drop in the development of new pressure ulcers during a patient’s stay in hospital. We are pleased that our patients are now routinely giving us patient satisfaction scores at the 99% level and that we have demonstrated our ability to save millions of dollars annually in health care spending that can help maintain the overall sustainability of our health care system.
Since it was implemented, our ACE Strategy has been recognized as a leading, innovative model in the care of older adults. In celebration and honour of our achievements, our ACE Strategy was awarded the 2014 3M Canada Healthcare Quality Team Award, the 2013 CERNER Canada Advancing Clinical Excellence Award for its IT Innovations, and was recognized in the Ontario Government’s 2013 Minister’s Medal Honouring Health, Quality and Safety. Three of the ACE Strategy’s individual models – the Maximizing Aging Using Volunteer Engagement Program, the Support Program for Caregivers of People with Dementia in 2012, and the ACE Unit in 2014 – have also been awarded Leading Practice designations by Accreditation Canada.
In 2016, the federally funded Canadian Foundation for Healthcare Improvement (CFHI) and the Canadian Frailty Network (CFN) announced their support to help launch the ACE Collaborative, allowing Mount Sinai Hospital staff to serve as a faculty in an international learning collaborative to provide 18 other hospitals from across Canada and Iceland with coaching and support towards launching ACE Strategy interventions at their own sites. With coaching, educational tools, workshops and supportive funding of $1 million, these hospitals have implemented over 50 new ACE Strategy models of care to suit the needs of their older patients with the hope that in the future they will support neighbouring organizations to do the same as well.
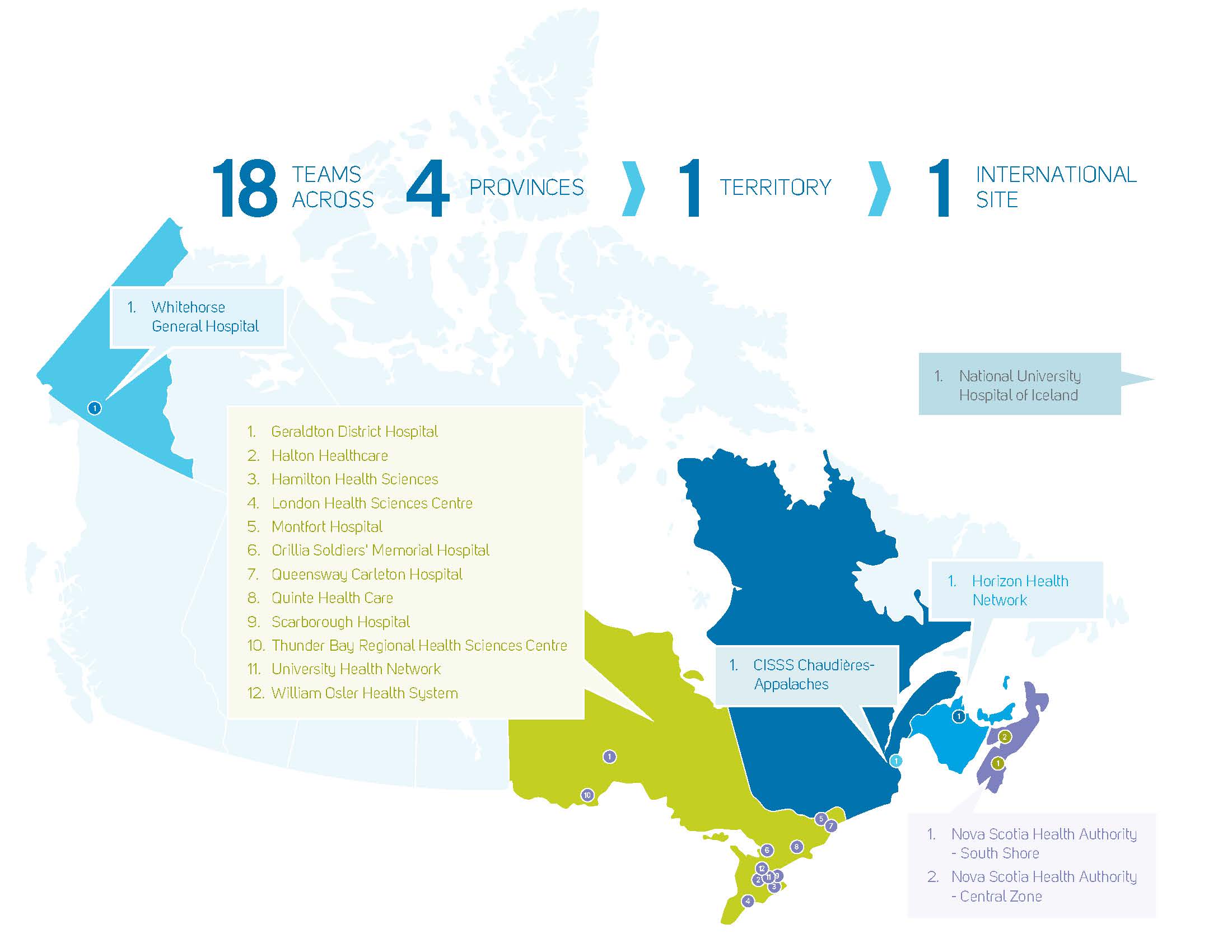
Most recently, in 2017, the Commonwealth Fund recognized the ACE Strategy as a leading international model of care that is ideally designed to meet the needs of complex patients.
Continuum of Care of Geriatrics Services
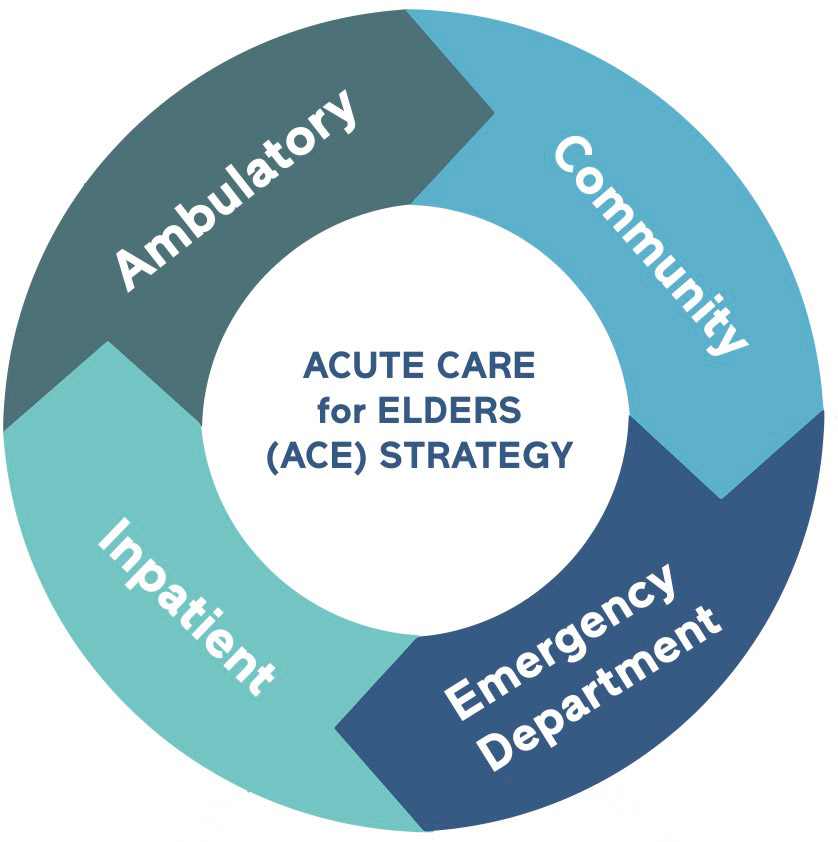
Outpatient Models
- Outpatient Geriatric Medicine, Geriatric Psychiatry & Palliative Medicine Clinics
- Telemedicine Clinics
Commnuity Models
- Home-Based Geriatric Primary/Specialty Care Program: House Calls
- Temmy Latner Home-Based Palliative Care Program
- Integrated Client Care Management Program
- Reitman Centre for Alzheimer’s Support and Caregiver Training
- Community and Staff Education Programs
- Community Paramedicine Program
- Community Outreach Team
Inpatient Models
- Geriatric Medicine, Geriatric Psychiatry & Palliative Medicine Consultation Services
- Orthogeriatrics Program
- Intensive Care Unit Geriatrics Program
- Safe Patients/Safe Staff
- ACE Unit
- ACE Unit Home Care Coordinator
- MAUVE Volunteer Program
- ACE Tracker
- Hospital at Home Program
ED Models
- ISAR Screening
- Geriatric Emergency Management (GEM) Nurses
- Geri-EM.com Staff Training Program
To learn more about each of the innovative services we provide, click on the links below:
Ambulatory
We provide a variety of clinic-based services for older adults who can benefit from them. Our geriatric medicine and psychiatry clinics provide comprehensive care to frail older adults who need the additional help of geriatric specialists. Under our ACE Strategy, these clinics are linked with the rest of our continuum of care to provide care to patients at risk of hospitalization or to others after a hospitalization to ensure their ongoing care needs are being met. We are also innovating in the provision of telemedicine services for homebound patients who could further benefit from this technology.
Community
Under our ACE Strategy, we have partnered with primary, home, community, and emergency medical care providers to deliver a variety of services that can enable older adults who could benefit from enhanced supports to age in place for as long as possible, avoid unnecessary hospitalizations, and to support their transition back home after a visit to our Emergency Department or a stay in hospital. Through our community-based programs, our initiatives help older adults remain active, engaged and independent members of their communities.
Emergency Department
When older adults are admitted to our Emergency Department (ED), some have particular care needs that can sometimes be overlooked and go unmet in this fast-paced environment. All of our ED Staff have received advanced training in geriatric care and our ED models of care have been redesigned to ensure that higher risk older adults are identified early and that all older patients receive the appropriate care they need. Under our ACE Strategy, we aim to help our patients to return home to live as independently as possible with improved connections to primary, home and community supports and our outpatient services.
Inpatient
Under our ACE Strategy, we have developed a number of inpatient models of care to ensure our frail older patients in particular receive holistic, person-centred elder-friendly care through an interprofessional approach when they are admitted to the hospital.
Date modified: June 2021

