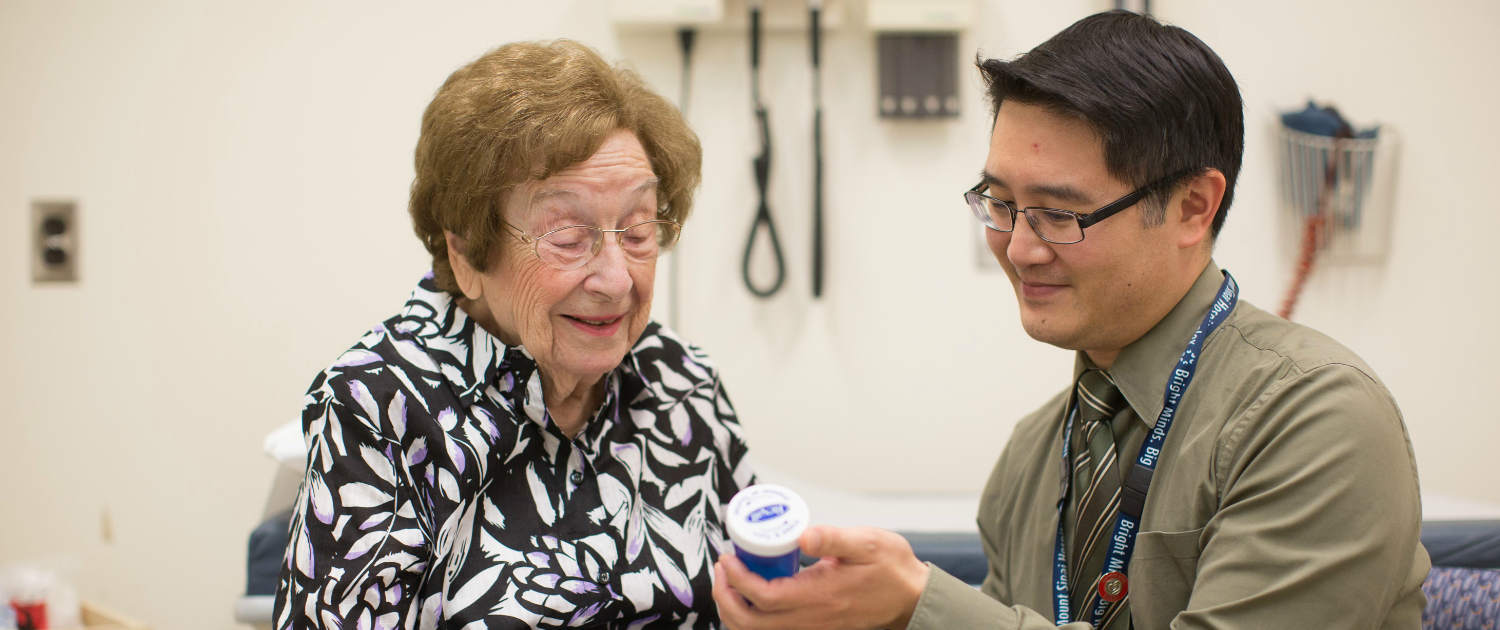
When older patients come to Mount Sinai Hospital for their care, they are often impressed to find pharmacists working closely alongside their doctors, nurses and therapists as equally essential members of a patient’s care team. So when the hospital launched its Healthy Ageing and Geriatrics Program in 2010, I was proud to be selected as Sinai Health System’s lead geriatrics pharmacist. In fact, our program remains the only one we know of in Canada where a Board Certified Geriatrics Pharmacist is a key member of the Inpatient Geriatric Medicine Consult Service and Outpatient Geriatric Medicine Clinics. I was further pleased that Rexall Canada recently provided our program the support of a second Geriatrics Pharmacist who helps assist our patients through our Community Outreach Team and other community-based programs as well.
Haven’t heard of a Board Certified Geriatrics Pharmacist (BCGP)? The geriatric specialty credential for pharmacists is the second largest specialty under the Board of Pharmacy Specialties in the United States, with almost 3,200 geriatric pharmacists worldwide. In Ontario, there are just over 300 BCGPs; I am part of a handful of them that practise in the hospital setting. With so many older patients requiring medication, one would think all pharmacists are specialists in geriatric care. Unfortunately, comprehensive geriatric education is not a mandatory part of pharmacy curriculum and post-graduate training in Canada. Nevertheless, I am proud to be sharing my knowledge and expertise with pharmacy students enrolled in a Geriatrics elective course at the University of Toronto’s Leslie Dan Faculty of Pharmacy. As well, I continue to mentor pharmacy students and hospital pharmacy residents that choose geriatric medicine as part of their experiential direct patient care rotations. So why should pharmacists become more essential members of our health care teams? As we age, we are likely to develop a number of chronic health conditions for which medication therapy will remain a core part of their treatment. Often, managing these health problems can mean that older adults may take many different medications. Managing several medications can be challenging.
There are many reasons why this is the case for some older adults. Health Literacy – a person’s ability to understand and communicate health information accurately – may be lower among older adults, which can reduce their adherence to treatment regimens. The lower health literacy of older adults also reduces their buy-in to the efficacy of the medication, which can be crucial because a patients’ beliefs and/or understanding about an illness and how medication therapy can help treat it plays a significant role in achieving positive health outcomes. Functional impairments, such as decreased visual acuity and manual dexterity, can make it difficult to understand how to take medications properly or make it physically challenging to access them. Other medical conditions, such as cognitive impairment and depression, are also predictors of suboptimal medication adherence. The odds of needing help with taking medications are greater among people with memory challenges. Serious side effects may occur from taking medications at the wrong time or in the wrong dose. Some older adults can put themselves at risk for experiencing drug-related problems if they don’t receive the assistance they may need.
Unfortunately, even if we reduced all these barriers to medications for older adults, there still wouldn’t be such a thing as a perfect medication therapy. Even when you take medications properly, they can still have some adverse (i.e. harmful) drug effects. These effects could range from less serious side effects such as a mild and temporary stomach ache to more serious things such as falls and a hospitalization.
While anyone taking a medication should be aware of the risks, older adults are particularly vulnerable to adverse drug effects. As you get older, your body changes. These changes can increase the chances that you’ll have side effects when you take medications. Older people usually have more health problems and take more medications than younger people. Because of this, they are also more likely to experience dangerous drug interactions. Every year, one in three adults 65 years of age or better has one or more adverse reactions to a medication. This is why it’s important for researchers to identify and help reduce the use of drugs that are associated with more risks than benefits in older people. Medication issues can often arise in many different situations, such as when new medicines are added or medicines are stopped, when a dose is changed, when medications are taken with alcohol and when non-prescription products are taken without the doctor or pharmacist knowing.
Integrating pharmacists within the health care teams of older patients is especially important when you consider that nearly 40 per cent of older Canadians are currently taking one inappropriate medication with an additional 12 per cent taking multiple inappropriate medications. Older Canadians further account for 57 per cent of all hospitalizations due to adverse drug events. However, with proper oversight from a pharmacist and a doctor, it is estimated that 40 per cent of harmful drug effects are preventable.